Excision of Cervical Rib through Supraclavicular Approach
Muhammad Sohail Umerani,Yahya Ashqan,Hira Burhan,Amjad Abdel Qader Darwish Hassan Rezwan Mohammed and Zahrah Alhaji
DOI10.21767/2380-7245.100163
Muhammad Sohail Umerani1*, Yahya Ashqan2, Hira Burhan3, Amjad Abdel Qader Darwish1, Hassan Rezwan Mohammed2 and Zahrah Alhaji2
1Department of Clinical Neurosciences, King Fahd Military Medical Complex, Dhahran, KSA
2Department of Vascular Surgery, King Fahd Military Medical Complex, Dhahran, KSA
3Dow University of Health Sciences, Karachi, Pakistan
- *Corresponding Author:
- Umerani, MS
Registrar Neurosurgeon
Department of Clinical Neurosciences
King Fahd Military Medical Complex
Dhahran, KSA
Tel: +966 565 978939
E-mail: drumerani@yahoo.com
Received Date: July 28, 2017; Accepted Date: August 10, 2017; Published Date: August 14, 2017
Citation: Umerani MS, Ashqan Y, Burhan H, Darwish AAQ, Mohammed HR, et al. (2017) Excision of Cervical Rib through Supraclavicular Approach. J Rare Disord Diagn Ther. 3:10. doi: 10.21767/2380-7245.100163
Abstract
Thoracic Outlet Syndrome (TOS) is a clinical condition due to compression of the neurovascular structures, such as brachial plexus and subclavian vessels, during their course between the neck and axilla. Different etiological factors including cervical rib are involved in this diverse group of disorder. Depending on these factors, patients presents with either neurological or vascular compromise. Multiple disciplinary team effort and appropriate surgical technique such as the supraclavicular approach to eliminate the definitive element defines cure in terms of long term functional capacity. We report a case of a 27 year old female who presented with complain of progressive left upper limb pain and paresthesias. We planned an excision of cervical rib with thrombectomy and stenting of the subclavian artery though a supraclavicular approach.
https://myseoblog.blogdon.net/
https://myseoblog.blogaaja.fi/
https://myseoblog.jimdosite.com/
https://myseoblog.edublogs.org/
https://myseoblog.websites.co.in/
https://myseoblog47.wordpress.com/
https://myseoblog.waarnnnnnnbenjij.nu/
https://myseoblog.jigsy.com/
https://szeith-rhounds-kliagy.yolasite.com/
https://myseoblog-40.webselfsite.net/
https://myseoblog.mystrikingly.com/
https://myseoblog.splashthat.com/
https://myseoblog.webnode.com.tr/
https://myseoblog.odoo.com/
https://myseoblog.creatorlink.net/
https://whiteseotr1-s-site.thinkific.com/
https://myseoblog.estranky.cz/
https://65390c7d9a166.site123.me/
https://myblogseoooo.blogspot.com/
https://myseoblog.hashnode.dev/
https://whiteseotr1.wixsite.com/myseoblog
https://myseoblogg.weebly.com/
https://sites.google.com/view/myseoblogg/
https://codepen.io/myseoblog/pens/public
https://myseoblogg.livejournal.com/
https://wakelet.com/@myseoblog87204
https://www.homify.com/users/9537482/myseoblog/
https://theomnibuzz.com/author/myseoblog/
https://lessons.drawspace.com/profile/323508/myseoblog/
https://my.desktopnexus.com/myseoblog/
https://writeupcafe.com/profile/myseoblog/
https://www.pearltrees.com/myseoblog
https://www.easyfie.com/myseoblog
https://pharmahub.org/members/27544
https://www.zupyak.com/u/myseoblog/posts
https://www.metroflog.co/myseoblog
https://www.fuzia.com/fz/myseoblog-myseoblog
https://tr.pinterest.com/whiteseotr1/
https://my.getjealous.com/myseoblog
https://micro.blog/myseoblog
https://www.tumblr.com/blog/myseobloggsblog
https://hub.docker.com/u/myseoblog
https://fire.blogfree.net/?act=Profile&MID=1342100
https://myseoblog.pixnet.net/blog
https://myseoblogg.seesaa.net/
https://www.threadless.com/@myseoblog/activity
https://neocities.org/site/myseoblog
https://myseoblog.amebaownd.com/
https://teletype.in/@myseoblog
https://ubl.xml.org/users/myseoblog S6t3Bh9Gwo
https://educatorpages.com/site/myseoblog/
https://myseoblog.onlc.fr/
Keywords
Thoracic outlet syndrome; Cervical rib; Supraclavicular approach
Introduction
Thoracic Outlet Syndrome (TOS) is an entrapment syndrome where major vessels and nerves of the upper extremity, while travelling from the thoraco-cervical region to the axilla, are compressed due to narrowing of the spaces in the thoracic outlet. A number of different anatomic or functional characteristics can be attributed to produce the symptoms during elevation of the upper limbs. Common etiologies include scaring of the scalenus anticus muscle because of previous trauma, costoclavicular, hyper abduction, cervical rib, fibrous bands and first thoracic rib. Patients with TOS usually present with neurogenic, venous, and/ or arterial symptoms [1-3]. The incidence of cervical ribs is 0.2% to 1.0% which is most often picked up incidentally on routine chest radiographs [4-7]. Most of these ribs are asymptomatic and necessitate no further management [8]. Gruber in 1869 was the first to describe cervical ribs [9]. He classified them into 4 types: In Type I the rib extends up to the transverse process of C7 whereas in type II it extends beyond the transverse process with no connection to the first thoracic rib. In type III it extends beyond the transverse process with partial fusion to the first rib by fibrous bands or cartilage and is seen completely fused to the first rib by a bony pseudo articulation in type IV. Type III and IV cervical ribs commonly lead to vascular compromise, including arterial compression, thrombosis, and aneurysm formation. About 95% of the patients have symptoms pertaining to neurogenic patients with venous TOS often presents acutely after either thrombosis of the subclavian vein or due to intermittent compression of the vein. Arterial TOS is the least common variety often presenting with acute or chronic secondary to aneurysm, occlusion, or embolization of the subclavian artery. These patients are frequently found to have bony abnormalities, such as cervical ribs or rudimentary ribs [10].
Different provocative tests can reproduce the symptoms. These include East test or "Hands-up" test, Adson or scalene maneuver, costoclavicular maneuver and Allen test. Doppler ultrasonography aids in the initial evaluation of the vascular flow through the compromised territory and distally. Helical Computed Tomography (CT) angiography can be diagnostic, to ascertain the extent of vascular compromise and also helps in establishing the adequacy of flow during the follow up course.
The initial plan of management conventionally is to continue conservative care where as surgical intervention is reserved in patients for acute vascular insufficiency, neurological dysfunction and pain refractory to conservative measures [11]. The surgical maneuver involves the release or removal of the confounding structures such as cervical rib excision, scalene muscle release, first rib resection and resection of fibro muscular bands [12].
Case Report
Thoracic Outlet Syndrome (TOS) is caused by impingement of the neurovascular structures passing through the thoracic inlet. We report a case of a 27 years old female who was referred to the Vascular Surgery Department of King Fahd Military Medical Complex from a peripheral hospital where she presented with complain of progressive left upper limb pain and paresthesias that started 4 weeks prior to presentation after elevating an object at home. The pain was gradually increasing in intensity more so with repeated movement of left arm at the shoulder joint. This was associated with left hand claudication and numbness. Initial workup showed left brachial artery thrombus for which she underwent brachial artery embolectomy. With this procedure her pain started improving but it did not subside and the numbness persisted in the left hand. She was thereafter shifted to our hospital after 10 days of initial procedure for further management.
On initial general examination, the patient is an average built, right handed lady sitting comfortably on the couch. A scar of previous surgical intervention was visible at the distal aspect of the left arm. Her left hand palmar surface was pale and cold on palpation. The capillary refilling was delayed with absent radial and brachial pulses, however with weak ulnar pulse. Neurologically she had normal left hand grip as compared to the right with a power of 5/5 in all muscle groups of left forearm and hand. There was no muscular atrophy with normal sensations and deep tendon reflexes. There was no restriction of movement at any of the joints in the left upper limb. Tip of left cervical rib was palpable with no cervical spine tenderness.
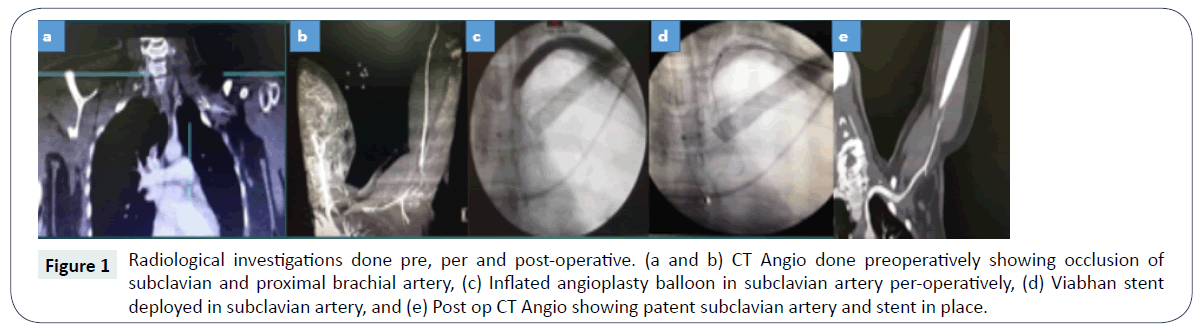
Laboratory investigations were unremarkable. Hand Doppler had shown no signals in radial and weak signals in ulnar and brachial arteries. CT angiogram revealed a filling defect measuring 40 x 11.5 mm at the second part of subclavian artery suggestive of thrombus due to cervical rib compression with non-visualized proximal segment of brachial artery (clavicle to the mid humerus), with narrowed and attenuated left axillary, brachial and radial arteries (Figure 1). Ulnar artery had normal caliber with no filling defect. Magnetic Resonance Imaging (MRI) of cervical spine and brachial plexus showed the left cervical rib crossing the left scalene triangle with no abnormal thickening or enhancement of the left brachial plexus nerve roots.
Figure 1: Radiological investigations done pre, per and post-operative. (a and b) CT Angio done preoperatively showing occlusion of subclavian and proximal brachial artery, (c) Inflated angioplasty balloon in subclavian artery per-operatively, (d) Viabhan stent deployed in subclavian artery, and (e) Post op CT Angio showing patent subclavian artery and stent in place.
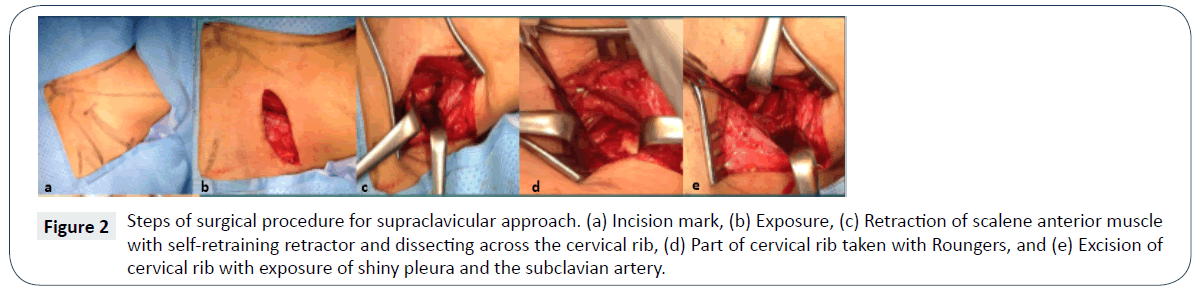
Thereafter patient and family members were counseled regarding our plan of excision of cervical rib with thrombectomy and stenting of the subclavian artery, to which they agreed. She underwent the above mentioned surgical procedure though a supraclavicular approach by the Neurosurgery team. Per operatively, a curvilinear incision in the supraclavicular region was given, and platysma opened. The phrenic nerve was identified on the surface of the anterior scalene muscle as it proceeds distally and was retracted medially with the anterior scalene muscle. Dissection was done up to the cervical rib which was identified compressing the vasculature, and excised along with release of the fibrous band (Figure 2). After excision of the rib, pulsations were visible in the previously compressed subclavian artery. Vascular surgery team performed catheter thromb-embolectomy of the axillary and brachial artery by Fogarty’s balloon catheter, followed by subclavian artery angioplasty and stenting through the left brachial artery with covered stent (Viabahn/Gore 7 mm x 5 cm) (Figure 1). Per operative angiogram showed recanalization of the hard organized thrombus in the subclavian artery, but the distal segments of both radial and ulnar arteries could not be recanalized. This was due to very hard, old organized thrombus which could be due to ongoing thrombo-embolic showers from the first surgery preoperatively. Trial of thrombolysis was done with Actylise (TPA) by direct intra-arterial infusion of 2 mg followed by 10 mg with no affect. Completion angiogram showed total occlusion of radial artery and distal occlusion of ulnar artery. The interroseous artery was patent and refilling of ulnar and radial artery was seen through the collaterals. Post-operative, the left hand pallor reduced and it became warm with capillary refill of less than 3 seconds. There were no neurological deficits and wound healing was good. Physiotherapy of the left upper extremity was planned to commence from 1st post-operative day for early pain free mobility. She was later discharged in a stable condition to be followed up in the clinic for post-operative radiological investigations. On follow up after 3 months patient is symptom free with warm hands, good capillary refilling and ulnar systolic pressure of 104 mmHg.
Figure 2: Steps of surgical procedure for supraclavicular approach. (a) Incision mark, (b) Exposure, (c) Retraction of scalene anterior muscle with self-retraining retractor and dissecting across the cervical rib, (d) Part of cervical rib taken with Roungers, and (e) Excision of cervical rib with exposure of shiny pleura and the subclavian artery.
Discussion
The term Thoracic Outlet Syndrome (TOS) was first used in 1956 to describe a symptom complex that resulted from compression of subclavian vessels and trunks of brachial plexus that travel from the thoracocervical region to the axilla coursing between the anterior and middle scalene muscle, through the costoclavicular space and under the pectoralis minor tendon [13]. Its prevalence was found to be 0.74% with higher rate in females as compared in males [14].
Two major types of TOS have been identified-vascular and neurogenic. The vascular type has been further divided into arterial or venous. Neurogenic TOS can be sub categorized into true or disputed. The former is accompanied by objective findings while the disputed form, which is more common, is not. 95% of the patients have a neurogenic form, while 2% have venous symptoms and only 1% has arterial compression [15]. Often patients present with symptoms indicative of more than one type. Common etiological factors producing these variable symptoms include cervical rib, fibrous bands, first thoracic rib and scalenus anticus muscle. Although in many cases no cause is identified [15].
Halsted in 1916 had studied a large series of 716 case reports with cervical ribs in which 125 had vascular symptoms and 27 had aneurysms distal to the point of compression by the rib and its attachments [16]. In 1934, Lewis and Pickering stated that trauma due to a cervical rib can lead to subclavian artery thrombosis and embolization [17]. Cervical rib anomaly is twice as common in women as men. It is present bilaterally in more than 50% of cases and asymptomatic in 90% of cases [18]. The fact that our patient had only the cervical rib as a sole factor compressing the major vascular structures causing TOS, as elucidated by history, physical examination and radiological evidences, therefore we opted for the supraclavicular approach to alleviate the symptoms. Our patient had Gruber Type III cervical rib that extended beyond the transverse process with fibrous bands attached to the first rib.
This along with Type IV commonly leads to vascular compromise, including arterial compression, thrombosis and aneurysm formation.
Complete cervical ribs have a 50% incidence of spontaneous onset of symptoms in neurogenic TOS as compared with 20% with incomplete ribs. On the contrary only complete ribs have been noted to produce arterial TOS.
A meticulous history and detailed neurovascular examination will guide to a probable diagnosis and also helps in distinguishing the type of TOS. Stress tests or provocative maneuvers form the basis of physical examination. The most common of these are the Adson's or scalene maneuvers. Others include East test or "Hands-up" test, costoclavicular maneuver and Allen test. They have very low specificity, sensitivity and predictive value [19]. Direct application of pressure on to the anterior scalene or upper segment of the pectoralis minor elicits focal stress test. A positive response is said if symptoms are reproduced within 15 to 30 s of application of the pressure. Some people use Tinel's sign, where percussing over the plexus reproduces symptoms.
X-ray cervical spine is done mostly as an initial investigation of choice that may demonstrates a cervical rib. Patients having arterial TOS were more likely to have cervical ribs on chest x-ray than patients with neurogenic or venous TOS [20]. Chest X-ray with apical lordotic views should be obtained to exclude a malignant lesion in the chest. Preoperative duplex ultrasound scanning demonstrates thrombosis or aneurysm of the vascular structure compromised with impediment of blood flow. It sometimes also detects compression missed by provocation test. This can serve as an important portable tool to evaluate the immediate post-operative status. Electromyography/nerve conduction velocity (EMG-NCV) study is not a routine investigation and is usually considered when a diagnosis of carpal or cubital tunnel syndrome is suspected. MRI scans of the cervical spine and brachial plexus are useful to exclude other possible differentials. CT scan of the area of the brachial plexus and apex of lung may be indicated. Helical 3D CT angiography has an edge over conventional techniques for determining the mechanism and site of compression especially in difficult cases [21].
Conservative treatment with postural control and physiotherapy is an acceptable initial plan of management, unless there is failure of conservative means (for 3-12 months), progressive neurological deficits, refractory pain, and acute or severe initial vascular insufficiency [22]. Arterial TOS has no non-surgical treatment and physical therapy in such an instance does not help. In 1863, Coote for the first time performed surgical removal of the left transverse process of 7th cervical vertebra to treat TOS [23]. More than a century later Brown and Charles worth published their data over 18 patients with 23 cervical ribs mentioning that resection of cervical rib was effective in improving their symptoms [24]. Fibrous bands should be removed along with cervical rib especially if they are tethering the plexus.
Prolonged arterial compression by a cervical rib results in subclavian aneurysm formation and thrombosis which necessitates further intervention in addition to cervical rib resection. This can be dealt in the form of Polytetrafluoroethylene (PTFE) or saphenous vein grafts [25]. On occasions thrombolysis or thrombectomy is considered obligatory in addition to a bypass in order to establish an effective arterial flow [26,27]. Instances where a subclavian artery stent placement is desired, it should be kept in mind that it must be placed after the cervical rib resection in order to secure the stent from being thrombosed from the rib compression [10].
The optimal surgical approach for the excision of rib removal has always been a topic of controversial debate. Popular ones are supraclavicular, transaxillary and infraclavicular but only the transaxillary and supraclavicular routes have coined their names. Earlier studies suggested that the transaxillary approach is appropriate only for first rib resection, and a supraclavicular approach is best when gaining access to the subclavian artery is desired along with cervical rib excision [28,29]. Now the transaxillary approach allows removal of both cervical and the first rib through a single incision site and a supraclavicular approach is indicated to allow access to the subclavian artery for aneurysm repair or to facilitate placement of a bypass graft [10]. The supraclavicular route has minimal risk to neurovascular structures during primary or secondary surgery. It allows the operating surgeon an excellent visualization of the entire brachial plexus, palpation of every structure, extensive micro neurolysis under the operating microscope, and room for appropriate nerve reconstruction, especially in cases of iatrogenic brachial plexus injury, after prior transaxillary first rib resection. A combination of supraclavicular and infraclavicular approach has also been suggested to allow for access to both the subclavian and axillary arteries [4,27]. Microsurgical neurovascular decompression of TOS without removal of the cervical or first rib using a supraclavicular approach has also proven its effectiveness for relief of neurological symptoms [30].
If neurological symptoms dominate than early surgical intervention in the course of the disease prevents degeneration of the brachial plexus and increases the effectiveness of postoperative physiotherapy [31]. Low cure rates have been attributed in certain cases due to longstanding intimal damage to the subclavian artery. This is secondary to a cervical rib fused to the first rib causing immense compression resulting in arterial injury. In these specific circumstances surgical removal of the cervical and first rib was ineffective.
Functional prognosis is the main factor in determining the outcome after surgical decompression. Post-operative management plays a pivotal role in establishing an early functional status of the extremity involved. Appropriate physical therapy for at least 3 months gives the desired practical response. Anticoagulation for a period of 3 to 6 months is to be continued depending upon the extent of vascular procedure [10].
In our case the use of thrombolysis is contraindicated due to recent surgery and the chronicity of the situation. The classic surgical repair was not ideal due to poor run off, and the decision for angioplasty and placing of a covered stent in order to cover the lesion of the subclavian artery and the chronic thrombus was chosen. We did not find any previous literature or case review describing a similar situation, and no trials of angioplasty for an organized arterial thrombosis; although it was extensively reported for cases of venous thrombosis and occlusion of IVC, and or iliac veins with or without the use of thrombolysis.
Conclusion
Although no single approach is novel but excision of the cervical rib through supraclavicular approach is not only simple but it also enables precise evaluation of the thoracic inlet and better exposure of the middle and upper trunks of the brachial plexus with release of confounding abnormal anatomical structures especially the cervical rib with minimal risk to the surrounding neurovascular structures. It also offers vascular surgeons the opportunity for conventional vascular repair. Since massive thrombo embolic shower may be amenable for the treatment, hence early diagnosis and management is crucial in TOS with an arterial component. Long term results are better with minimal complications and patients are able to function independently with their daily activities.
References
- Thompson RW, Petrinec D (1997) Surgical treatment of thoracic outlet compression syndromes: diagnostic considerations and transaxillary first rib resection. Ann Vasc Surg 11: 315-323.
- Fugate MW, Rotellini-Coltvet L, Freischlag JA (2009) Current management of thoracic outlet syndrome. Curr Treat Options Cardiovasc Med 11: 176-183.
- Sanders RJ, Hammond SL, Rao NM (2008) Thoracic outlet syndrome: a review. Neurologist 14: 365-373.
- Davidovic LB, Kostic DM, Jakovljevic NS, Kuzmanovic IL, Simic TM (2003) Vascular thoracic outlet syndrome. World J Surg 27: 545-550.
- Makhoul RG, Machleder HI (1992) Developmental anomalies at the thoracic outlet: an analysis of 200 consecutive cases. J Vasc Surg 16: 534-542.
- Guttentag AR, Salwen JK (1999) Keep your eyes on the ribs: the spectrum of normal variants and diseases that involve the ribs. Radiographics 19: 1125-1142.
- Adson AW, Coffey JR (1927) Cervical rib: a method of anterior approach for relief of symptoms by division of the scalenus anticus. Ann Surg 85: 839-857.
- Davies AH, Walton J, Stuart E, Morris PJ (1991) Surgical management of the thoracic outlet compression syndrome. Br J Surg 78: 1193-1195.
- Gruber W (1869) Ueber die Halsrippen des Menschen, mít vergleíchendanatomischen Bemerkungen. Mém Acad Sci 2: 7-27.
- Chang KZ, Likes K, Davis K (2013) The significance of cervical ribs in thoracic outlet syndrome. J Vasc Surg 57: 771-775.
- Bisschop P (2003) Nerve lesions and entrapment neuropathies of the upper limb in a system of orthopedic medicine
- Efstathopoulos D, Spridonos S, Aretaiou P, Seitaridis S, Dimitriadis A, et al. (2002) Our experience of surgical treatment of thoracic outlet syndrome. Orthopedic Proceedings: Hellenic Assciation of Orthopedic Surgery and Traumatology (HAOST) Thessaloniki, Greece pp: 22-27.
- Peet RM, Hendricksen JD, Guderson TP, Martin GM (1956) Thoracic outlet syndrome: evaluation of a therapeutic exercise program. Mayo Clin Proc 31: 281-287.
- Brewin J, Hill M, Ellis H (2009) The prevalence of cervical ribs in a London population. Clin Anat 22: 331-336.
- Bhattacharya V, Hansrani M, Wyatt MG, Lambert D, Jones NA (2003) Outcome following surgery for thoracic outlet syndrome. Eur J Vasc Endovasc Surg 26: 170-175.
- Halsted WS (1916) An experimental study of circumscribed dilation of an artery immediately distal to a partially occluding band, and its bearing on dilatation of the subclavian artery observed in certain cases of cervical rib. J Exp Med 24: 271-286.
- Lewis T, Pickering GW (1934) Observations upon maladies in which blood supply to digist ceases intermittently or permanently, and upon bilateral gangrene or digits. Clin Sci 1: 327.
- Sanders RJ, Haug CE (1991) Thoracic outlet syndrome: a common sequel of neck injuries. Philadelphia: JB Lippincott 40: 129-185.
- Nord KM, Kapoor P, Fisher J (2008) False positive rate of thoracic outlet syndrome diagnostic maneuvers. Electromyogr Clin Neurophysiol 48: 67-74.
- Orlando MS, Likes KC, Mirza S, Cao Y, Cohen A, et al. (2015) A decade of excellent outcomes after surgical intervention in 538 patients with thoracic outlet syndrome. J Am Coll Surg 220: 934-939.
- Hasanadka R, Towne JB, Seabrook GR (2007) Computed tomography angiography to evaluate thoracic outlet neurovascular compression. Vasc Endovascular Surg 41: 316-321.
- Degeorges R, Reynaud C, Becquemin JP (2004) Thoracic outlet syndrome surgery: long-term functional results. Ann Vasc Surg 18: 558-565.
- Coote H (1861) Exostosis of the left transverse process of the seventh cervical vertebra surrounded by blood vessels and nerves. Lancet 1: 360-361.
- Brown SC, Charlesworth D (1988) Results of excision of a cervical rib in patients with the thoracic outlet syndrome. Br J Surg 75: 431-433.
- Gelabert HA, Machleder HI (1997) Diagnosis and management of arterial compression at the thoracic outlet. Ann Vasc Surg 11: 359-366.
- Bearn P, Patel J, O’Flynn WR (1993) Cervical ribs: a cause of distal and cerebral embolism. Postgrad Med J 69: 65-68.
- Davidovic LB, Koncar IB, Pejkic SD, Kuzmanovic IB (2009) Arterial complications of thoracic outlet syndrome. Am Surg 75: 235-239.
- Sanders RJ, Hammond SL (2002) Management of cervical ribs and anomalous first ribs causing neurogenic thoracic outlet syndrome. J Vasc Surg 36: 51-56.
- Nannapaneni R, Marks SM (2003) Neurogenic thoracic outlet syndrome. Br J Neurosurg 17: 144-148.
- Rochkind S, Shemesh M, Patish H, Graif M, Segev Y, et al. (2007) Thoracic outlet syndrome: a multidisciplinary problem with a perspective for microsurgical management without rib resection. Acta Neurochir Suppl 100: 145-147.
- Al-Hashel JY, El Shorbgy AA, Ahmed SF (2013) Early versus late surgical treatment for neurogenic thoracic outlet syndrome. ISRN Neurol pp: 1-6.
Open Access Journals
- Aquaculture & Veterinary Science
- Chemistry & Chemical Sciences
- Clinical Sciences
- Engineering
- General Science
- Genetics & Molecular Biology
- Health Care & Nursing
- Immunology & Microbiology
- Materials Science
- Mathematics & Physics
- Medical Sciences
- Neurology & Psychiatry
- Oncology & Cancer Science
- Pharmaceutical Sciences