Rapidly Progressive Plummer Vinson Syndrome
Michael Skolka and Helen Pauly-Hubbard
DOI10.21767/2380-7245.100059
Michael Skolka and Helen Pauly-Hubbard*
Penn State Hershey College of Medicine, Hershey, PA, USA
- *Corresponding Author:
- Helen Pauly-Hubbard
Penn State Hershey College of Medicine
500 University Drive, Hershey, PA-17033, USA
Tel: 215-407-9922
E-mail: hpaulyhubbard@pennstatehealth.psu.edu
Received date: May 01, 2017; Accepted date: May 11, 2017; Published date: May 17, 2017
Citation: Skolka M, Pauly-Hubbard H. Rapidly Progressive Plummer Vinson Syndrome. J Rare Disord Diagn Ther. 2017, 3:6. doi: 10.21767/2380-7245.100059
Copyright: © 2017 Skolka M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Context: Plummer Vinson Syndrome is diagnosed by a triad of dysphagia, esophageal webs, and iron deficiency anemia. These symptoms typically progress over a period of six months and often include other systemic effects such as angular cheilitis, glossitis, and spooning of the fingernails. Treatment includes iron supplementation as well as esophageal dilation. Annual upper endoscopic surveillance is an important measure for cancer surveillance.
Case report: A 47-year-old African American female with a history of hypertension presented to the emergency room with dysphagia. Over a period of two weeks, the patient first noticed difficulty swallowing large chunks of food followed shortly by trouble swallowing liquids. She described pain in her oropharynx with eating and regurgitated both solids and liquids every time she ate. She had lost 10 pounds over two weeks and described a new craving for ice (pica). Review of systems was otherwise negative. She denied chest pain, dyspnea, abdominal pain, hematemesis, and had no history of reflux. Physical exam was unremarkable. There was no evidence of glossitis, angular cheilitis, or spooning of the nail beds (koilonychia).
Conclusion: This case represents an atypical or rapid progression of Plummer Vinson Syndrome which developed over a period of approximately two weeks. Subsequently, the patient did not display the tell-tale systemic effects typically associated with this syndrome. Clinicians should be aware of similar presentations that fulfill the diagnostic criteria but circumvent the typical progression and associated sequelae. Indeed, recognizing this triad has important implications for esophageal cancer surveillance.
Keywords
Plummer Vinson syndrome; Dysphagia; Iron deficiency
Case Report
A 47-year-old African American female with a history of hypertension presented to the emergency room with dysphagia. Over a period of two weeks, the patient first noticed difficulty swallowing large chunks of food followed shortly by trouble swallowing liquids. She described pain in her oropharynx with eating and regurgitated both solids and liquids every time she ate. She had lost 10 pounds over two weeks and described a new craving for ice (pagophagia). Review of systems was otherwise negative. She denied chest pain, dyspnea, abdominal pain, hematemesis, and had no history of Gastroesophageal Reflux Disease (GERD). Physical exam was unremarkable. There was no evidence of glossitis, angular cheilitis, or spooning of the nail beds (koilonychia).
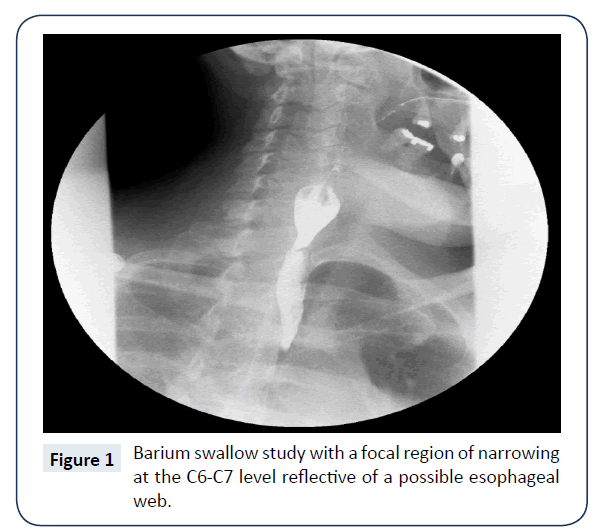
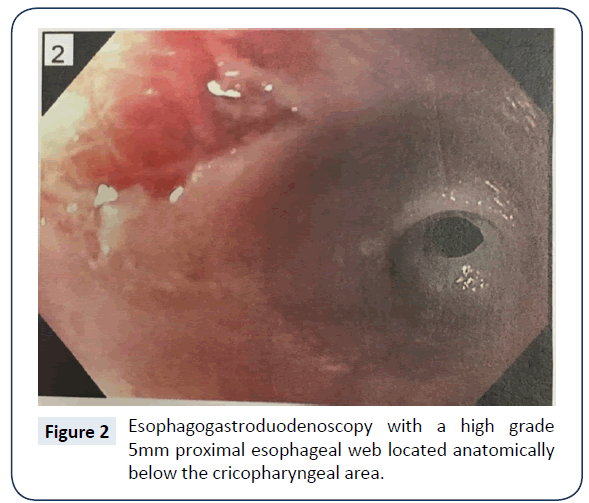
Initial studies included a CBC which showed a microcytic anemia with Hgb 6.5 g/dL, Hct 24.1%, MCV 59.2fl, MCHC 27.0%, and RDW 19.2%. An iron panel confirmed anemia secondary to iron deficiency with a serum iron of 14 μg/L, ferritin 7 μg/L, TIBC 402 μg/dL, and iron saturation 3%. The patient was admitted to the hospital and transfused. A barium swallow study was then ordered for dysphagia (Figure 1), which displayed a probable esophageal web at C6-C7. An Esophagogastroduodenoscopy (EGD) was then performed, which confirmed the presence of a 5.0 mm esophageal web (Figure 2). The web was dilated to 10.0 mm via balloon. Plummer Vinson Syndrome (PVS) was diagnosed. After the procedure, the patient quickly resumed oral intake without difficulty. The patient was discharged on omeprazole, ferrous sulfate, and Vitamin C and instructed to follow-up with the gastroenterologist.
Discussion and Conclusion
The diagnostic criteria for PVS, also known as Paterson-Brown- Kelly syndrome, include a triad of esophageal webs, dysphagia, and iron deficiency anemia [1]. This rare disease typically progresses over a period of six months and affects primarily women in their fourth to seventh decade of life [2]. Associated symptoms include fatigue, pallor, glossitis, angular cheilitis, and koilonychia secondary to anemia. PVS is thought to be autoimmune in nature [1]. Treatment begins with iron supplementation, which has been shown to resolve dysphagia in many patients, while others require mechanical dilation of esophageal webs [3]. Symptom resolution following successful balloon dilation, as performed in this patient, has also been described [4]. Patients are at an increased risk for pharyngeal and esophageal squamous cell carcinoma and require an annual EGD for follow up. However, a reduction in mortality with annual surveillance has not been confirmed [5].
This case is an atypical presentation of PVS due to the rapid progression of symptoms over a period of two weeks. Subsequently, most likely because of the brief and rapid course, this patient did not display many of the tell-tale systemic effects of iron deficiency anemia typically observed in PVS such as glossitis, angular cheilitis, or koilonychia. The patient did, however, complain of pagophagia or pica.
In summary, PVS is a rare triad composed of common symptoms seen often in medicine. Clinicians should consider this syndrome when a patient presents with dysphagia and symptoms of anemia. Indeed, recognizing the triad has important implications for cancer surveillance, and diagnostic work-up. Lastly, physicians should be aware of atypical presentations that fulfill the diagnostic criteria but circumvent the typical progression and associated sequelae.
References
- Novacek G (2006) Plummer-Vinson syndrome. Orphanet J Rare Dis1: 36.
- Dinler G, Tander B, Kalayci AG, Rizalar R (2009) Plummer-Vinson syndrome in a 15-year-old boy. Turk J Pediatr 51: 384-386.
- Hoffmann RM, Jaffe PE (1995) Plummer-Vinson syndrome. A case report and literature review. Arch Intern Med 155: 2008-2111.
- Sreenivas DV, Kumar A, Mannar R, Babu GR (2002) Results of Savary-Gilliard Dilatation in the management of cervical web of esophagus. Hepato-Gastroenterology 49: 188-190.
- Demirci F, Savas MC, Kepkep N, Okan V, Yilmaz M, et al. (2005) Plummer-Vinson syndrome and dilation therapy: a report of two cases. Turk J Gastroenterol 16: 224-227.
Open Access Journals
- Aquaculture & Veterinary Science
- Chemistry & Chemical Sciences
- Clinical Sciences
- Engineering
- General Science
- Genetics & Molecular Biology
- Health Care & Nursing
- Immunology & Microbiology
- Materials Science
- Mathematics & Physics
- Medical Sciences
- Neurology & Psychiatry
- Oncology & Cancer Science
- Pharmaceutical Sciences