Approach To Dorsal Nasal Sinus: A Rare Case Report
Mukta Verma and Arun K Singh
DOI10.21767/2380-7245.100179
Mukta Verma* and Arun K Singh
Department of Plastic Surgery, King George’s Medical University, Lucknow, Uttar Pradesh, India
- *Corresponding Author:
- Mukta Verma
Department of Plastic Surgery
King George’s Medical University
Lucknow, Uttar Pradesh, India
Tel: + 9451738117
E-mail: drmukta23@gmail.com
Received Date: May 14, 2018; Accepted Date: May 28, 2018; Published Date: June 04, 2018
Citation: Verma M, Singh AK (2018) Approach To Dorsal Nasal Sinus: A Rare Case Report. J Rare Disord Diagn Ther. 4:11. doi: 10.21767/2380-7245.100179
Abstract
Congenital midline dorsal nasal sinus is a rare clinical presentation in our day today clinical practice. Complete surgical excision can cure the patient. We must be careful while taking decision regarding its surgical management as it may have an intracranial extension and neurosurgical consultation and craniotomy may be required. Here we are discussing our case with the comprehensive approach and review of available literature.
https://marsbahislinki.com https://marsbetgiris.com https://mobilebahiss.com https://1xbetsgirisi.com https://onwinegiris.com https://betistegiris.com https://piacasinogiris.com https://holiganbahiss.com https://holiganbetting.com https://girisholigan.com https://mostbetegiris.com https://mariobetoyna.com https://meritgirisi.com https://meritkinge.com https://kingmerite.com https://nanogiris.com https://casinoplusa.com https://casinoplusgiris.com https://betriyal.net https://pluscasinogiris.com
Keywords
Dorsal nasal sinus; Midline; Excision; Intracranial; Rare
Introduction
Usually midline dorsal nasal sinus is a sign of underlying dermoid cyst [1]. They have a unique embryological origin. Other midline nasal masses may be gliomas and encephaloceles which may have an intracranial connection [2,3].
The common differential diagnoses of a midline nasal mass may include inflammatory lesions, traumatic deformity, benign neoplasms, malignant neoplasms and congenital masses. The purpose of this case report is to discuss about the clinical presentation, pathogenesis, diagnosis and surgical management of this rare congenital anomaly.
Case Report
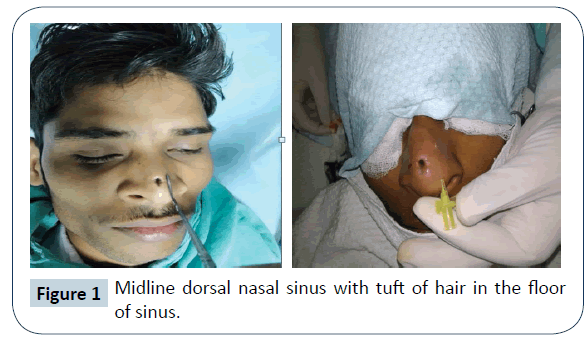
A 23 years, young male patient presented to our out-patient department with history of an opening over dorsum of nose with tuft of hair in it since his childhood. He also complained of on and off white color discharge from that opening but there was no history of nasal obstruction. He had been operated in his childhood for the same complaint but did not get relief of his symptoms. On examination, there was a sinus tract of approx 1.5 cm x 0.5 cm size over dorsum of the nose, extending from the supratip region to mid-dorsum. White discharge (foul smelling cheesy material) could be expressed from the sinus opening. Surrounding skin was normal in colour and texture. There was no other apparent congenital anomaly. Anterior rhinoscopy findings were normal on both the sides. MRI was suggestive of a midline anterior nasal sinus tract with no intranasal and intracranial extension.
Management
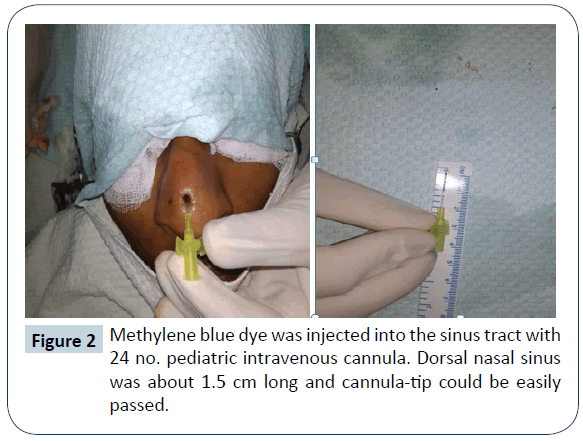
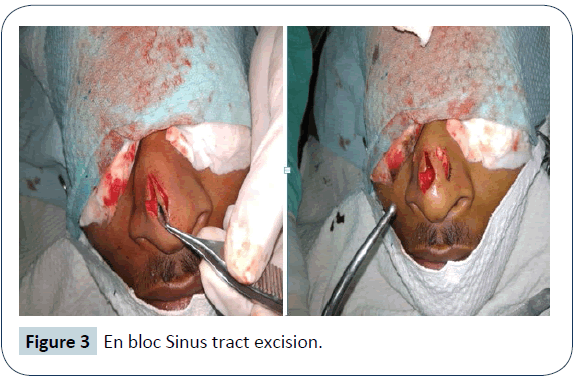
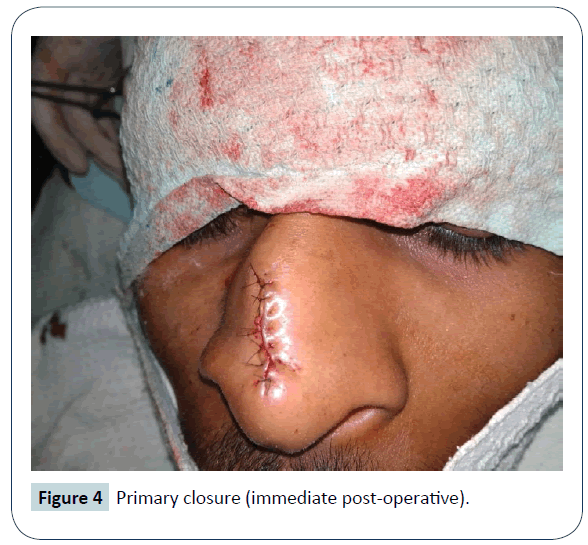
Surgical excision of the sinus tract was planned under local anaesthesia as there was no intracranial extension as suggested by MRI scan. Lidocaine HCl 2% and epinephrine 1: 100,000 injections were used to provide local anesthesia and vasoconstriction in the operative field. Methylene blue dye was injected in the sinus tract and metallic probe was passed in the sinus tract to guide the complete excision of the sinus tract. At first, an elliptical incision was given around the sinus tract opening and then it was extended towards the radix. The blind dilated end of sinus tract was reaching upto the nasal bones. It was filled with hair and cheesy foul smelling discharge. After complete excision, wound was irrigated with providone iodine solution and normal saline and closure was done using nylon 5-0. Excised sinus tract was sent for histopathological examination and it came out to be a dermoid sinus cyst. Patient was discharged about two hours after surgical procedure with advice of effective elevation of head for about 24 hours to avoid post operative edema and pain. Post operative recovery was uneventful and sutures were removed on post operative day five. Wound healed with good linear scar. There was no recurrence of symptoms for about 1 year of follow up (Figures 1- 4).
Discussion
Nasal dermoid is a rare developmental anomaly of nose. Nasal dermoid can present as a cyst, a sinus, a fistula and may have intracranial extension [4]. Incidence is estimated at 1:20,000 to 1:40,000 births [2,3]. Though there are no syndromes associated with the development of midline nasal dermoid cyst, congenital anomalies have been reported in association with these lesions in up to 41% of cases [5]. These include other craniofacial abnormalities such as hypertelorism, cleft lip and palate, hemifacial microsomia and aural atresia, as well as defects including hydrocephalus, branchial sinuses, albinism, cardiac, gastrointestinal, genital and CNS anomalies. Pathogenesis involve incomplete obliteration of of neuroectoderm in developing frontonasal region [6]. Unlike epidermoid cysts, which are purely ectodermal, dermoid cysts contain both ectodermal and mesodermal elements, including adnexal structures and sebaceous glands [3,7]. In contrast to teratomas, they contain no endodermally derived structures. Midline dorsal nasal cyst may present as a nasal mass, pit or fistula located anywhere from the glabella to columella. Although the majority of lesions are superficial with no deep extension, a variably reported percentage may end blindly within the deeper midline structures of the nose or extend intracranially [1,5,7,8]. Hair protruding from the punctum is pathognomonic of dermoid cysts [5]. Rarely, multiple openings can be present and midline cysts may exist at more than one level on the nose and glabella [4]. They may secrete sebaceous material and can become intermittently inflamed or infected. Sequelae of infection can result in osteomyelitis, meningitis or cerebral abscess. These complications may also result from inadequate surgical excision [1]. Biopsy/ FNAC of such lesions with an intracranial connection can lead to meningitis or cerebrospinal fluid leak. Surgical strategy depends on the location and extent of the lesion, ranging from local excision via an open or endoscopic approach to a combined transcranial approaches. Surgical excision by midline vertical incision is the common approach [9-11]. Other approaches includes transverse incision, lateral rhinotomy and external rhinoplasty [1,5,7,8,12].
Conclusion
Dorsal nasal sinus is a rare congenital anomaly of nose. A careful pre-operative evaluation is required to rule out any intracranial extension of the sinus tract. Complete surgical excision is the key to avoid the recurrence of symptoms.
Conflict of Interest
Authors are declared that there is no conflict of interest.
References
- Yavuzer R, Bier U, Jackson IT (1999) Be careful: it might be a nasal dermoid cyst. Plast Reconstr Surg 103: 2082-2083.
- Pratt LW (1965) Midline cysts of the nasal dorsum: embryologic origin and treatment. Laryngoscope 75: 968-80.
- Hughes GB, Sharpino G, Hunt W, Tucker HM (1980) Management of the congenital midline nasal mass: a review. Head Neck Surg 2: 222-233.
- Sessions RB (1982) Nasal dermal sinuses: new concepts and explanations. Laryngoscope 92: 1-28.
- Denoyelle F, Ducroz V, Roger G, Garabedian EN (1997) Nasal dermoid sinus cysts in children. Laryngoscope 107: 795-800.
- Weiss DD, Robson CD, Mulliken JB (1998) Transnasal endoscopic excision of midline nasal dermoid from the anterior cranial base. Plast Reconstr Surg 102: 2119-2123.
- Rohrich RJ, Lowe JB, Schwartz MR (1999) The role of open rhinoplasty in the management of nasal dermoid cysts. Plast Reconstr Surg 104: 1459-1466.
- Morrissey MS, Bailey CM (1991) External rhinoplasty approach for nasal dermoids in children. Ear Nose Throat J 70: 445-449.
- Uglietta JP, Boyko OB, Rippe DJ, Fuller GN, Schiff SJ, et al. (1989) Intracerebral extension of nasal dermoid cyst: CT appearance. J Comput Assist Tomogr 13: 1061-1064.
- Fornadley JA, Tami TA (1989) The use of magnetic resonance imaging in the diagnosis of the nasal dermal sinus-cyst. Otolaryngol Head Neck Surg 101: 397-398.
- Brunner H, Harned JW (1942) Dermoid cysts of the dorsum of the nose. Arch Otolaryngol 36: 86-94.
- Posnick JC, Bortoluzzi P, Armstrong DC, Drake JM (1994) Intracranial nasal dermoid sinus cysts: computed tomographic scan findings and surgical results. Plast Reconstr Surg 93: 745-754.
Open Access Journals
- Aquaculture & Veterinary Science
- Chemistry & Chemical Sciences
- Clinical Sciences
- Engineering
- General Science
- Genetics & Molecular Biology
- Health Care & Nursing
- Immunology & Microbiology
- Materials Science
- Mathematics & Physics
- Medical Sciences
- Neurology & Psychiatry
- Oncology & Cancer Science
- Pharmaceutical Sciences